I. ETHICS
A. Ethics: The branch of philosophy concerned with the distinction between right and wrong on the basis of a body of knowledge, not only on the basis of opinions
B. Morals: Behavior in accordance with customs or tradition, usually reflecting personal or religious beliefs
C. Ethical principles: Codes that director govern nursing actions
D. Values: Beliefs and attitudes that may influence behavior and the process of decision making
E. Values clarification: Process of analyzing one’s own values to understand oneself more completely regarding what is truly important
F. Ethical codes
1. Ethical codes provide broad principles for determining and evaluating client care.
2. These codes are not legally binding, but the board of nursing has authority in most states to reprimand nurses for unprofessional conduct that results from violation of the ethical codes.
3. Specific ethical codes are as follows:
- The Code of Ethics for Nurses developed by the International Council of Nurses; Website: http://www.icn.ch/about-icn/code-of-ethicsfor-nurses/.
- The American Nurses Association Code of Ethics can be viewed on the American Nurses Association Web site: http://www. nursingworld.org/codeofethics.
G. Ethical dilemma
- An ethical dilemma occurs when there is a conflict between 2 or more ethical principles.
- No correct decision exists, and the nurse must make a choice between 2 alternatives that are equally unsatisfactory.
- Such dilemmas may occur as a result of differences in cultural or religious beliefs.
- Ethical reasoning is the process of thinking through what one should do in an orderly and systematic manner to provide justification for actions based on principles; thenurseshouldgatherallinformationtodeterminewhetheranethicaldilemmaexists, examine his or her own values, verbalize the problem, consider possible courses of action, negotiate the outcome, and evaluate the action taken.
H. Advocate
- An advocate is a person who speaks up for or acts on the behalf of the client, protects the client’s right to make his or her own decisions, and upholds the principle of fidelity.
- An advocate represents the client’s viewpoint to others.
- An advocate avoids letting personal values influence advocacy for the client and supports the client’s decision, even when it conflicts with the advocate’s own preferences or choices.
I. Ethics committees
- Ethics committees take an interprofessional approach to facilitate dialogue regarding ethical dilemmas.
- These committees develop and establish policies and procedures to facilitate the prevention and resolution of dilemmas. An important nursing responsibility is to act as a client advocate and protect the client’s rights.
II. REGULATION OF NURSING PRACTICE
A. Nurse Practice Act
- A nurse practice act is a series of statutes that have been enacted by each state legislature to regulate the practice of nursing in that state.
- Nurse practice acts set educational requirements for the nurse, distinguish between nursing practice and medical practice, and define the scope of nursing practice.
- Additional issues covered by nurse practice acts include licensure requirements for protection of the public, grounds for disciplinary action, rights of the nurse licensee if a disciplinary action is taken, and related topics.
- All nurses are responsible for knowing the provisions of the act of the state or province in which they work.
B. Standards of care
- Standards of care are guidelines that identify what the client can expect to receive in terms of nursing care.
- The guidelines determine whether nurses have performed duties in an appropriate manner.
- If the nurse does not perform duties within accepted standards of care, the nurse places himself or herself in jeopardy of legal action.
- If the nurse is named as a defendant in a malpractice lawsuit and proceedings show that the nurse followed neither the accepted standards of care outlined by the state or province nurse practice act nor the policies of the employing institution, the nurse’s legal liability is clear; he or she is liable.
C. Employee guidelines
- Respondent superior: The employer is held liable for any negligent acts of an employee if the alleged negligent act occurred during the employment relationship and was within the scope of the employee’s responsibilities.
- Contracts
- Nurses are responsible for carrying out the terms of a contractual agreement with the employing agency and the client.
- The nurse-employee relationship is governed by established employee handbooks and client care policies and procedures that create obligations, rights, and duties between those parties.
- Institutional policies
- Written policies and procedures of the employing institution detail how nurses are to perform their duties.
- Policies and procedures are usually specific and describe the expected behavior on the part of the nurse.
- Although policies are not laws, courts generally rule against nurses who violate policies.
- If the nurse practices nursing according to client care policies and procedures established by the employer, functions within the job responsibility, and provides care consistently in a nonnegligent manner, the nurse minimizes the potential for liability.
The nurse must follow the guidelines identified in the Nurse Practice Act and agency policies and procedures when delivering client care.
D. Hospital staffing
- Charges of abandonment may be made against nurses who “walk out” when staffing is inadequate.
- Nurses in short staffing situations are obligated to make a report to the nursing administration.
E. Floating
- Floating is an acceptable practice used by health care facilities to alleviate understaffing and overstaffing.
- Legally, the nurse cannot refuse to float unless a union contract guarantees that nurses can work only in a specified area or the nurse can prove lack of knowledge for the performance of assigned tasks.
- Nurses in a floating situation must not assume responsibility beyond their level of experience or qualification.
- Nurses who float should inform the supervisor of any lack of experience in caring for the type of clients on the new nursing unit.
- A resource nurse who is skilled in the care of clients on the unit should also be assigned to the float nurse; in addition, the float nurse should be given an orientation of the unit and the standards of care for the unit should be reviewed (the float nurse can care for “overflow” clients whose acuity level more closely match the nurses’ experience).
F. Disciplinary action
1. Boards of nursing may deny, revoke, or suspend any license to practice as a registered nurse, according to their statutory authority.
2. Some causes for disciplinary action are as follows:
- Unprofessional conduct
- Conduct that could affect the health and welfare of the public adversely
- Breach of client confidentiality
- Failure to use sufficient knowledge, skills, or nursing judgment
- Physically or verbally abusing a client
- Assuming duties without sufficient preparation
- Knowingly delegating to unlicensed personnel nursing care that places the client at risk for injury
- Failure to maintain an accurate record for each client
- Falsifying a client’s record
- Leaving a nursing assignment without properly notifying appropriate personnel
III. Legal Liability
A. Laws
1. Nurses are governed by civil and criminal law in roles as providers of services, employees of institutions, and private citizens.
2. The nurse has a personal and legal obligation to provide a standard of client care expected of a reasonably competent professional nurse.
3. Professional nurses are held responsible (liable) for harm resulting from their negligent acts or their failure to act.
B. Types of laws
- Contract Law - concerned with enforcement of agreements among private individuals.
- Civil Law - concerned with relationships among persons and the protection of a person’s rights. Violation may cause harm to an individual or property, but no grave threat to society exists.
- Criminal Law - concerned with relationships between individuals and governments, and with acts that threaten society and its order; a crime is an offense against society that violates a law and is defined as a misdemeanor (less serious nature) or felony (serious nature).
- Tort Law - a civil wrong, other than a breach in contract, in which the law allows an injured person to seek damages from a person who caused the injury.
C. Negligence and malpractice
- Negligence is conduct that falls below the standard of care.
- Negligence can include acts of commission and acts of omission.
- The nurse who does not meet appropriate standards of care may be held liable.
- Malpractice is negligence on the part of the nurse.
- Malpractice is determined if the nurse owed a duty to the client and did not carry out the duty and the client was injured because the nurse failed to perform the duty.
- Proof of liability
- Duty: At the time of injury, a duty existed between the plaintiff and the defendant.
- Breach of duty: The defendant breached duty of care to the plaintiff.
- Proximate cause: The breach of the duty was the legal cause of injury to the client.
- Damage or injury: The plaintiff experienced injury or damages or both and can be compensated by law.
Examples of Negligent Acts:
- Medication errors that result in injury to the client
- Intravenous administration errors, such as incorrect flow rates or failure to monitor a flow rate, that result in injury to the client
- Falls that occur as a result of failure to provide safety to the client
- Failure to use sterile technique when indicated
- Failure to check equipment for proper functioning
- Burns sustained by the client as a result of failure to monitor bath temperature or equipment
- Failure to monitor a client’s condition
- Failure to report changes in the client’s condition to the health care provider
- Failure to provide a complete report to the oncoming nursing staff
D. Professional liability insurance
- Nurses need their own liability insurance for protection against malpractice lawsuits.
- Having their own insurance provides nurses protection as individuals; this allows the nurse to have an attorney, who has only the nurse’s interests in mind, present if necessary.
E. Good Samaritan laws
- State legislatures pass Good Samaritan laws, which may vary from state to state.
- These laws encourage health care professionals to assist in emergency situations and limit liability and offer legal immunity for persons helping in an emergency, if they give reasonable care.
- Immunity from suit applies only when all conditions of the state law are met, such as that the health care provider (HCP) receives no compensation for the care provided and the care given is not intentionally negligent.
F. Controlled substances
- The nurse should adhere to facility policies and procedures concerning administration of controlled substances, which are governed by federal and state laws.
- Controlled substances must be kept locked securely, and only authorized personnel should have access to them.
- Controlled substances must be properly signed out for administration and a correct inventory must be maintained.
IV. Collective Bargaining
A. Collective bargaining is a formalized decision-making process between representatives of management and representatives of labor to negotiate wages and conditions of employment.
B. When collective bargaining breaks down because the parties cannot reach an agreement, the employees may call a strike or take other work actions.
C. Striking presents a moral dilemma to many nurses because nursing practice is a service to people.
V. Legal Risk Areas
A. Assault
1. Assault occurs when a person puts another person in fear of a harmful or offensive contact.
2. The victim fears and believes that harm will result because of the threat.
B. Battery is an intentional touching of another’s body without the other’s consent.
C. Invasion of privacy includes violating confidentiality, intruding on private client or family matters, and sharing client information with unauthorized persons.
D. False imprisonment
- False imprisonment occurs when a client is not allowed to leave a health care facility when there is no legal justification to detain the client.
- False imprisonment also occurs when restraining devices are used without an appropriate clinical need.
- A client can sign an Against Medical Advice form when the client refuses care and is competent to make decisions.
- The nurse should document circumstances in the medical record to avoid allegations by the client that cannot be defended.
E. Defamation is a false communication that causes damage to someone’s reputation, either in writing (libel) or verbally (slander).
F. Fraud results from a deliberate deception intended to produce unlawful gains.
- There may be exceptions to certain legal risks areas, such as assault, battery, and false imprisonment, when caring for a client with a mental health disorder experiencing acute distress who poses a risk to himself or herself or others. In this situation, the nurse must assess the client to determine loss of control and intervene; accordingly, the nurse should use the least restrictive methods initially, but then use interventions such as restraint if the client’s behavior indicates the need for this intervention.
VI. Client’s Rights
A. Description
1. The client’s rights document, also called the Client’s (Patient’s) Bill of Rights, reflects acknowledgment of a client’s right to participate in her or his health care with an emphasis on client autonomy.
2. The document provides a list of the rights of the client and responsibilities that the hospital cannot violate.
- Right to considerate and respectful care
- Right to be informed about diagnosis, possible treatments, and likely outcome, and to discuss this information with the health care provider
- Right to know the names and roles of the persons who are involved in care
- Right to consent or refuse a treatment
- Right to have an advance directive
- Right to privacy
- Right to expect that medical records are confidential
- Right to review the medical record and to have information explained
- Right to expect that the hospital will provide necessary health services
- Right to know if the hospital has relationships with outside parties that may influence treatment or care
- Right to consent or refuse to take part in research
- Right to be told of realistic care alternatives when hospital care is no longer appropriate
- Right to know about hospital rules that affect treatment, and about charges and payment methods
3. The client’s rights protect the client’s ability to determine the level and type of care received; all health care agencies are required to have a Client’s Bill of Rights posted in a visible area.
4. Several laws and standards pertain to client’s rights.
B. Rights for the mentally ill
1. The Mental Health Systems Act created rights for mentally ill people.
2. The Joint Commission has developed policy statements on the rights of mentally ill people.
3. Psychiatric facilities are required to have a Client’s Bill of Rights posted in a visible area.
- Rights for the Mentally Ill
- Right to be treated with dignity and respect
- Right to communicate with persons outside the hospital
- Right to keep clothing and personal effects with them
- Right to religious freedom
- Right to be employed
- Right to manage property
- Right to execute wills
- Right to enter into contractual agreements
- Right to make purchases
- Right to education
- Right to habeas corpus (written request for release from the hospital)
- Right to an independent psychiatric examination
- Right to civil service status, including the right to vote
- Right to retain licenses, privileges, or permits
- Right to sue or be sued
- Right to marry or divorce
- Right to treatment in the least restrictive setting
- Right not to be subject to unnecessary restraints
- Right to privacy and confidentiality
- Right to informed consent
- Right to treatment and to refuse treatment
- Right to refuse participation in experimental treatments or research
C. Organ donation and transplantation
- A client has the right to decide to become an organ donor and a right to refuse organ transplantation as a treatment option.
- An individual who is at least 18 years old may indicate a wish to become a donor on his or her driver’s license (state-specific) or in an advance directive.
- The Uniform Anatomical Gift Act provides a list of individuals who can provide informed consent for the donation of a deceased individual’s organs.
- The United Network for Organ Sharing sets the criteria for organ donations.
- Some organs, such as the heart, lungs, and liver, can be obtained only from a person who is on mechanical ventilation and has suffered brain death, whereas other organs or tissues can be removed several hours after death.
- A donor must be free of infectious disease and cancer.
- Requests to the deceased’s family for organ donation usually are done by the HCP or nurse specially trained for making such requests.
- Donation of organs does not delay funeral arrangements; no obvious evidence that the organs were removed from the body shows when the body is dressed; and the family incurs no cost for removal of the organs donated.
D. Religious beliefs: Organ donation and transplantation
- Catholic Church: Organ donation and transplants are acceptable.
- Orthodox Church: Church discourages organ donation.
- Islam (Muslim) beliefs: Body parts may not be removed or donated for transplantation.
- Jehovah’s Witness: An organ transplant may be accepted, but the organ must be cleansed with a nonblood solution before transplantation.
- Orthodox Judaism
- All body parts removed during autopsy must be buried with the body because it is believed that the entire body must be returned to the earth; organ donation may not be considered by family members.
- Organ transplantation may be allowed with the rabbi’s approval.
VII. Informed Consent
A. Description
- Informed consent is the client’s approval (or that of the client’s legal representative) to have his or her body touched by a specific individual.
- Consents, or releases, are legal documents that indicate the client’s permission to perform surgery, perform a treatment or procedure, or give information to a third party.
- Types of Consent.
- Admission Agreement - are obtained at the time of admission and identify the health care agency’s responsibility to the client.
- Immunization Consent - may be required before the administration of certain immunizations; the consent indicates that the client was informed of the benefits and risks of the immunization.
- Blood Transfusion Consent - indicates that the client was informed of the benefits and risks of the transfusion. Some clients hold religious beliefs that would prohibit them from receiving a blood transfusion, even in a life-threatening situation.
- Surgical Consent - is obtained for all surgical or invasive procedures or diagnostic tests that are invasive. The health care provider, surgeon, or anesthesiologist who performs the operative or other procedure is responsible for explaining the procedure, its risks and benefits, and possible alternative options.
- Research Consent- obtains permission from the client regarding participation in a research study. The consent informs the client about the possible risks, consequences, and benefits of the research.
- Special Consents - are required for the use of restraints, photographing the client, disposal of body parts during surgery, donating organs after death, or performing an autopsy.
- Informed consent indicates the client’s participation in the decision regarding health care.
- The client must be informed, in understandable terms, of the risks and benefits of the surgery or treatment, what the consequences are for not, treatment options, and the name of the health care provider performing the surgery or procedure.
- A client’s questions about the surgery or procedure must be answered before signing the consent.
- A consent must be signed freely by the client without threat or pressure and must be witnessed (the witness must be an adult).
- A client who has been medicated with sedating medications or any other medications that can affect the client’s cognitive abilities must not be asked to sign a consent.
- Legally, the client must be mentally and emotionally competent to give consent.
- If a client is declared mentally or emotionally incompetent, the next of kin, appointed guardian (appointed by the court), or durable power of attorney for health care has legal authority to give consent.
- Mentally or Emotionally Incompetent Clients:
- Declared incompetent
- Unconscious
- Under the influence of chemical agents such as alcohol or drugs
- Chronic dementia or other mental deficiency that impairs thought processes and ability to make decisions
- A competent client 18 years of age or older must sign the consent.
- In most states, when the nurse is involved in the informed consent process, the nurse is witnessing only the signature of the client on the informed consent form.
- An informed consent can be waived for urgent medical or surgical intervention as long as institutional policy so indicates.
- A client has the right to refuse information and waive the informed consent and undergo treatment, but this decision must be documented in the medical record.
- A client may withdraw consent at any time.
An informed consent is a legal document, and the client must be informed by the HCP (i.e., physician, surgeon), in understandable terms, of the risks and benefits of surgery, treatments, procedures, and plan of care. The client needs to be a participant in decisions regarding health care.
B. Minors
1. A minor is a client under legal age as defined by state statute (usually younger than 18 years).
2. A minor may not give legal consent, and consent must be obtained from a parent or the legal guardian; assent by the minor is important because it allows for communication of the minor’s thoughts and feelings.
3. Parental or guardian consent should be obtained before treatment is initiated for a minor except in the following cases: in an emergency; in situations in which the consent of the minor is sufficient, including treatment related to substance abuse, treatment of a sexually transmitted infection, human immunodeficiency virus (HIV) testing and acquired immunodeficiency syndrome (AIDS) treatment, birth control services, pregnancy, or psychiatric services; the minor is an emancipated minor; or a court order or other legal authorization has been obtained.
C. Emancipated minor
1. An emancipated minor has established independence from his or her parents through marriage, pregnancy, or service in the armed forces, or by a court order.
2. An emancipated minor is considered legally capable of signing an informed consent.
VIII. Health Insurance Portability and Accountability Act
A. Description
1. The Health Insurance Portability and Accountability Act (HIPAA) describes how personal health information (PHI) may be used and how the client can obtain access to the information.
2. PHI includes individually identifiable information that relates to the client’s past, present, or future health; treatment; and payment for health care services.
3. The act requires health care agencies to keep PHI private, provides information to the client about the legal responsibilities regarding privacy, and explains the client’s rights with respect to PHI. 4. The client has various rights as a consumer of health care under HIPAA, and any client requests may need to be placed in writing; a fee may be attached to certain client requests. 5. The client may file a complaint if the client believes that privacy rights have been violated.
B. Client’s rights include the right to do the following:
- Inspect a copy of PHI.
- Ask the health care agency to amend the PHI that is contained in a record if the PHI is inaccurate.
- Request a list of disclosures made regarding the PHI as specified by HIPAA.
- Request to restrict how the health care agency uses or discloses PHI regarding treatment, payment, or health care services, unless information is needed to provide emergency treatment.
- Request that the health care agency communicate with the client in a certain way or at a certain location; the request must specify how or where the client wishes to be contacted. 6. Request a paper copy of the HIPAA notice.
C. Health care agency use and disclosure of PHI
1. The health care agency obtains PHI while providing or administering health insurance benefits.
2. Use or disclosure of PHI may be done for the following:
- Health care payment purposes
- Health care operations purposes
- Treatment purposes
- Providing information about health care services
- Data aggregation purposes to make health care benefit decisions
- Administering health care benefits
3. Additional uses of PHI disclosures
- Compliance with legal proceedings or for limited law enforcement purposes
- To a family member or significant other in a medical emergency
- To a personal representative appointed by the client or designated by law
- For research purposes in limited circumstances
- To a coroner, medical examiner, or funeral director about a deceased person
- To an organ procurement organization in limited circumstances
- To avert a serious threat to the client’s health or safety or the health or safety of others
- To a governmental agency authorized to oversee the health care system or government programs
- To the Department of Health and Human Services for the investigation of compliance with the Health Insurance Portability and Accountability Act or to fulfill another lawful request
- To federal officials for lawful intelligence or national security purposes
- To protect health authorities for public health purposes
- To appropriate military authorities if a client is a member of the armed forces
- In accordance with a valid authorization signed by the client
IX. Confidentiality/Information Security
A. Description
1. In the health care system, confidentiality/information security refers to the protection of privacy of the client’s PHI.
2. Clients have a right to privacy in the health care system.
3. A special relationship exists between the client and nurse, in which information discussed is not shared with a third party who is not directly involved in the client’s care.
4. Violations of privacy occur in various ways
- Taking photographs of the client
- Release of medical information to an unauthorized person, such as a member of the press, family, friend, or neighbor of the client, without the client’s permission
- Use of the client’s name or picture for the health care agency’s sole advantage
- Intrusion by the health care agency regarding the client’s affairs
- Publication of information about the client or photographs of the client, including on a social networking site
- Publication of embarrassing facts
- Public disclosure of private information
- Leaving the curtains or room door open while a treatment or procedure is being performed
- Allowing individuals to observe a treatment or procedure without the client’s consent
- Leaving a confused or agitated client sitting in the nursing unit hallway
- Interviewing a client in a room with only a curtain between clients or where conversation can be overheard
- Accessing medical records when unauthorized to do so
B. Nurse’s responsibility
1. Nurses are bound to protect client confidentiality by most nurse practice acts, by ethical principles and standards, and by institutional and agency policies and procedures.
2. Disclosure of confidential information exposes the nurse to liability for invasion of the client’s privacy.
3. The nurse needs to protect the client from indiscriminate disclosure of health care information that may cause harm
Maintenance of Confidentiality:
- Not discussing client issues with other clients or staff uninvolved in the client’s care
- Not sharing health care information with others without the client’s consent (includes family members or friends of the client and social networking sites)
- Keeping all information about a client private, and not revealing it to someone not directly involved in care
- Discussing client information only in private and secluded areas
- Protecting the medical record from all unauthorized readers
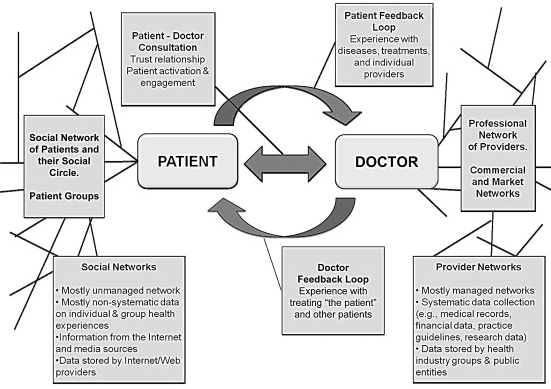
C. Social networks and health care
D. Medical records
1. Medical records are confidential.
2. The client has the right to read the medical record and have copies of the record.
3. Only staff members directly involved in care have legitimate access to a client’s record; these may include HCPs and nurses caring for the client, technicians, therapists, social workers, unit secretaries, client advocates, and administrators (e.g., for statistical analysis, staffing, quality care review). Others must ask permission from the client to review a record.
D. Social Networking and Health Care
- Specific social networking sites can be beneficial to health care providers (HCPs) and clients; misuse of social networking sites by the HCP can lead to Health Insurance Portability and Accountability Act (HIPAA) violations and subsequent termination of the employee.
- Nurses need to adhere to the code of ethics, confidentiality rules, and social media rules. Additional information about these codes and rules can be located at the American Nurses Association Web site at http://www.nursingworld. org/Functional Menu Categories/About ANA/Social-Media/ Social-Networking-Principles-Toolkit.
- Standards of professionalism need to be maintained and any information obtained through any nurse-client relationship cannot be shared in any way.
- The nurse is responsible for reporting any identified breach of privacy or confidentiality.
D. Medical records
- Medical records are confidential.
- The client has the right to read the medical record and have copies of the record.
- Only staff members directly involved in care have legitimate access to a client’s record; these may include HCPs and nurses caring for the client, technicians, therapists, social workers, unit secretaries, client advocates, and administrators (e.g., for statistical analysis, staffing, quality care review). Others must ask permission from the client to review a record.
- The medical record is stored in the records or the health information department after discharge of the client from the health care facility.
E. Information technology/computerized medical records
- Health care employees should have access only to the client’s records in the nursing unit or work area.
- Confidentiality/information security can be protected by the use of special computer access codes to limit what employees have access to in computer systems.
- The use of a password or identification code is needed to enter and sign off a computer system.
- A password or identification code should never be shared with another person.
- Personal passwords should be changed periodically to prevent unauthorized computer access.
F. When conducting research, any information provided by the client is not to be reported in any manner that identifies the client and is not to be made accessible to anyone outside the research team.
The nurse must always protect client confidentiality.
X. Legal Safeguards
A. Risk management
1. Risk management is a planned method to identify, analyze, and evaluate risks, followed by a plan for reducing the frequency of accidents and injuries.
2. Programs are based on a systematic reporting system for incidents or unusual occurrences.
B. Incident reports
- The incident report is used as a means of identifying risk situations and improving client care.
- Follow specific documentation guidelines.
- Fill out the report completely, accurately, and factually.
- The report form should not be copied or placed in the client’s record.
- Make no reference to the incident report form in the client’s record.
- The report is not a substitute for a complete entry in the client’s record regarding the incident.
- If a client injury or error in care occurred, assess the client frequently.
- The health care provider must be notified of incident and the client’s condition.
C. Safeguarding valuables
- Client’s valuables should be given to a family member or secured for safekeeping in a stored and locked designated location, such as the agency’s safe; the location of the client’s valuables should be documented per agency policy.
- Many health care agencies require a client to sign a release to free the agency of the responsibility for lost valuables.
- A client’s wedding band can be taped in place unless a risk exists for swelling of the hands or fingers.
- Religious items, such as medals, may be pinned to the client’s gown if allowed by agency policy.
D. HCP’s prescriptions
1. The nurse is obligated to carry out an HCP’s prescription except when the nurse believes a prescription to be inappropriate or inaccurate.
2. The nurse carrying out an inaccurate prescription may be legally responsible for any harm suffered by the client.
3. If no resolution occurs regarding the prescription in question, the nurse should contact the nurse manager or supervisor.
4. The nurse should follow specific guidelines for telephone prescriptions.
5. The nurse should ensure that all components of a medication prescription are documented.
- Components of a Medication Prescription:
- Date and time prescription was written
- Medication name ▪ Medication dosage
- Route of administration
- Frequency of administration
- Health care provider’s signature
- Telephone Prescription Guidelines:
- Date and time the entry.
- Repeat the prescription to the health care provider (HCP), and record the prescription.
- Sign the prescription; begin with “t.o.” (telephone order), write the HCP’s name, and sign the prescription.
- If another nurse witnessed the prescription, that nurse’s signature follows.
- The HCP needs to countersign the prescription within a time frame according to agency policy.
The nurse should never carry out a prescription if it is unclear or inappropriate. The HCP should be contacted immediately.
E. Documentation
1. Documentation is legally required by accrediting agencies, state licensing laws, and state nurse and medical practice acts.
2. The nurse should follow agency guidelines and procedures. Do's and Don'ts:
- Use a black-colored ink pen for narrative documentation.
- Date and time entries.
- Provide objective, factual, and complete documentation.
- Document care, medications, treatments, and procedures as soon as possible after completion.
- Document client responses to interventions.
- Document consent for or refusal of treatments.
- Document calls made to other health care providers.
- Use quotes as appropriate for subjective data.
- Use correct spelling, grammar, and punctuation.
- Sign and title each entry.
- Follow agency policies when an error is made (i.e., draw 1 line through the error, initial, and date).
- Follow agency guidelines regarding late entries.
- Use only the user identification code, name, or password for computerized documentation.
- Maintain privacy and confidentiality of documented information printed from the computer.
- Do not document for others or change documentation for other individuals. ▪ Do not use unacceptable abbreviations.
- Do not use judgmental or evaluative statements, such as “uncooperative client.”
- Do not leave blank spaces on documentation forms.
- Do not lend access identification computer codes to another person; change password at regular intervals.
F. Client and family teaching
- Provide complete instructions in a language that the client or family can understand.
- Document client and family teaching, what was taught, evaluation of understanding, and who was present during the teaching.
- Inform the client of what could happen if information shared during teaching is not followed.
XI. Advance Directives
A. Client (Patient) Self-Determination Act
- The Client (Patient) Self-Determination Act is a law that indicates clients must be provided with information about their rights to identify written directions about the care that they wish to receive if they become incapacitated and are unable to make health care decisions.
- On admission to a health care facility, the client is asked about the existence of an advance directive, and if one exists, it must be documented and included as part of the medical record; if the client signs an advance directive at the time of admission, it must be documented in the client’s medical record.
- The 2 basic types of advance directives include instructional directives and durable power of attorney for health care.
- Instructional directives: Lists the medical treatment that a client chooses to omit or refuse if the client becomes unable to make decisions and is terminally ill.
- Durable power of attorney for health care: Appoints a person (health care proxy) chosen by the client to make health care decisions on the client’s behalf when the client can no longer make decisions.
B. Do not resuscitate (DNR) orders
- A DNR order should be written if the client and health care provider have made the decision that the client’s health is deteriorating, and the client chooses not to undergo cardiopulmonary resuscitation if needed.
- The client or his or her legal representative must provide informed consent for the DNR status.
- The DNR order must be defined clearly so that other treatment, not refused by the client, will be continued.
- Some states offer DNR Comfort Care and DNR Comfort Care Arrest protocols; these protocols list specific actions that HCPs will take when providing cardiopulmonary resuscitation (CPR).
- All health care personnel must know whether a client has a DNR order; if a client does not have a DNR order, HCPs need to make every effort to revive the client.
- A DNR order needs to be reviewed regularly according to agency policy and may need to be changed if the client’s status changes.
- DNR protocols may vary from state to state, and it is important for the nurse to know his or her state’s protocols.
C. The nurse’s role
- Discussing advance directives with the client opens the communication channel to establish what is important to the client and what the client may view as promoting life versus prolonging dying.
- The nurse needs to ensure that the client has been provided with information about the right to identify written directions about the care that the client wishes to receive.
- On admission to a health care facility, the nurse determines whether an advance directive exists and ensures that it is part of the medical record; the nurse also offers information about advance directives if the client indicates he or she wants more information.
- The nurse ensures that the HCP is aware of the presence of an advance directive.
- All health care workers need to follow the directions of an advance directive to be safe from liability.
- Some agencies have specific policies that prohibit the nurse from signing as a witness to a legal document, such as an instructional directive.
- If allowed by the agency, when the nurse acts as a witness to a legal document, the nurse must document the event and the factual circumstances surrounding the signing in the medical record; documentation as a witness should include who was present, any significant comments by the client, and the nurse’s observations of the client’s conduct during this process.
XII. Reporting Responsibilities
- Nurses are required to report certain communicable diseases or criminal activities such as child or elder abuse or domestic violence; dog bite or other animal bite, gunshot or stab wounds, assaults, and homicides; and suicides to the appropriate authorities.
B. Impaired nurse
- If the nurse suspects that a co-worker is abusing chemicals and potentially jeopardizing a client’s safety, the nurse must report the individual to the nursing supervisor/nursing administration in a confidential manner. (Client safety is always the first priority.)
- Nursing administration notifies the board of nursing regarding the nurse’s behavior.
- Many institutions have policies that allow for drug testing if impairment is suspected.
C. Occupational Safety and Health Act (OSHA)
- OSHA requires that an employer provide a safe workplace for employees according to regulations.
- Employees can confidentially report working conditions that violate regulations.
- An employee who reports unsafe working conditions cannot be retaliated against by the employer.
D. Sexual harassment
- Sexual harassment is prohibited by state and federal laws.
- Sexual harassment includes unwelcome conduct of a sexual nature.
- Follow agency policies and procedures to handle reporting a concern or complaint.






